The Role of PRP Injections in Joint Pain Management
Managing joint pain often involves a multifaceted approach tailored to an individual’s specific condition and health goals. As medical science advances, new options become available for patients and their physicians to explore. One area of growing interest is the use of biologic treatments, which utilize substances derived from the body itself. Platelet-rich plasma, or PRP, is one such option. PRP injections use a patient’s own blood components as part of a comprehensive pain management strategy.
What Are PRP Injections?
Platelet-rich plasma is a preparation derived directly from a patient’s own blood. Platelets are small cell fragments known for their high concentration of proteins called growth factors. These are involved in the body’s natural healing processes.
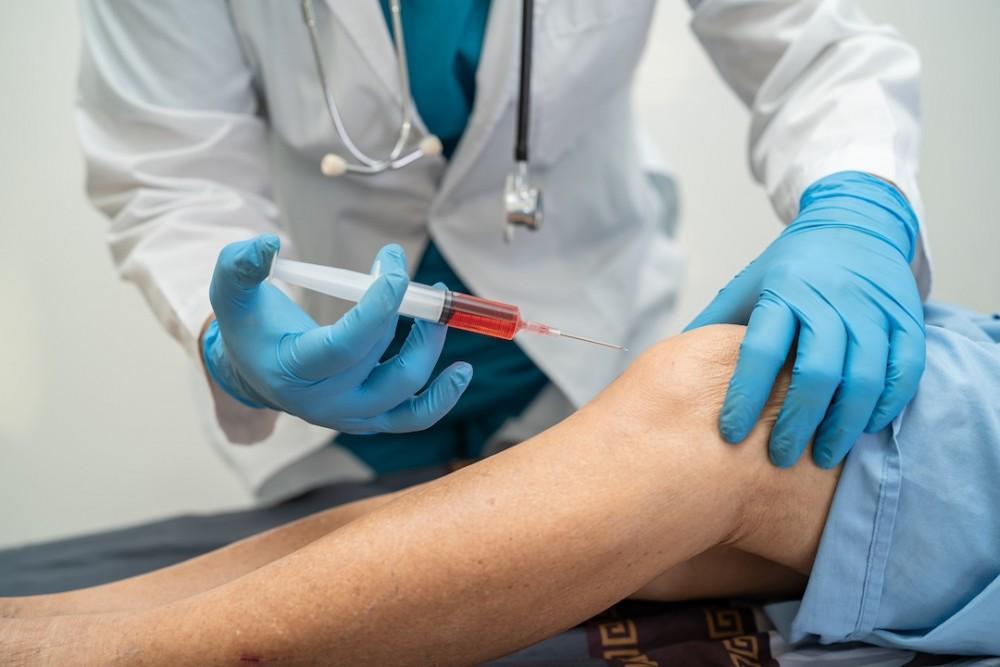
The process of creating PRP begins with a standard blood draw from the patient’s arm. This blood sample is then placed into a centrifuge to separate the blood into its different components based on their density. Through this process, the platelets are isolated and concentrated within a small volume of plasma. The resulting liquid, platelet-rich plasma, contains a much higher concentration of platelets than is found in regular blood. This substance is then prepared for injection.
How Do They Work?
The conceptual mechanism behind PRP injections centers on the function of platelets and the growth factors they contain. They release growth factors that act as signals, initiating a cascade of cellular responses designed to repair damaged tissue. By injecting a concentrated form of these platelets directly into a painful joint, the goal is to augment the body’s natural reparative signals in that specific location. The introduction of these growth factors potentially supports cellular repair activities.
What Should You Expect?
Outcomes following PRP injections can differ widely among individuals. For some, the procedure is followed by a period of symptom relief or improvements in joint function over time. Others may experience less noticeable changes.
After the injection, mild soreness, swelling, or discomfort at the site is sometimes reported and tends to resolve within several days. Some individuals notice benefits within weeks, while for others, the impact may be subtle or emerge over a longer period. Recovery timelines and the number of treatments needed are highly individualized, shaped by the specific joint involved and each person’s overall health profile.
It is helpful to maintain open communication with your healthcare provider about your experiences and to follow recommended activity modifications or physical therapy when advised. Clarity about the expected course and the recognition that responses vary can support realistic planning and better decision-making about ongoing care. Detailed discussions with your clinician about potential risks, alternative treatments, and your personal history are recommended as you assess the possible role of PRP within your broader pain management strategy.
Seek Professional Pain Management
Navigating the options for joint pain requires guidance from a qualified specialist. A professional with experience in pain management can conduct a thorough evaluation, which includes reviewing your medical history, performing a physical examination, and discussing your treatment goals. This comprehensive assessment is the foundation for developing a personalized care plan.
3 Benefits of an Early Diagnosis for Gut Issues